Feb 18, 2021 · accumulating evidence supports ending isolation and precautions for persons with covid-19 using a symptom-based strategy. specifically, researchers have reported that people with mild to moderate covid-19 remain infectious no longer than 10 days after their symptoms began, and those with more severe illness or those who are severely immunocompromised remain infectious no longer than 20 days. How to write medical soap notes. in the medical worls, "soap" stands for subjective, objective, assessment and plan. the soap note is a daily notation of a patient's condition, progress and immediate plan for diagnosis and treatment. a well. It’s a patient’s right to view his or her medical records, receive copies of them and obtain a summary of the care he or she received. the process for doing so is straightforward. when you use the following guidelines, you can learn how to. Her clinical experience includes working as a medical assistant for a network of rural health clinics, and as a medical coder, insurance claims specialist, and medical records auditor. she worked as a medical office manager for ten years, where she recruited and trained all medical assistants.
• the “soap” note o s = subjective (what the patient tells you) o o = objective (info from pe, labs, radiology) o a = assessment (dx and ddx) o p = plan (treatment, further tests, etc. ) • discharge summary o narrative in format o summarizes the events of a hospital stay o subjective terminology is used. Hospitals, pharmacies and other health care institutions maintain patients’ medical records. these institutions also issue patients copies of transaction documents for the medical expenses. it's important to record and maintain these docume.

Whether you're interested in reviewing information doctors have collected about you or you need to verify a specific component of a past treatment, it can be important to gain access to your medical records online. this guide shows you how. The soap note (an acronym for subjective, objective, assessment, and plan) is a method of documentation employed by healthcare providers to write out notes in a patient 's chart, along with other common formats, such as the admission note. Consumer's rights with respect to their medical records hhs hipaa home for individuals soap for medical records your medical records this guidance remains in effect only to the extent that it is consistent with the court’s order in ciox health, llc v. azar, no.
The advent of electronic medical records has not only changed the format of medical records but has increased accessibility of files. the use of an individual dossier style medical record, where records are kept on each patient by name and illness type originated at the mayo clinic out of a desire to simplify patient tracking and to allow for. Jan 27, 2021 · medical records often contain highly sensitive and private information. only specific individuals have access to your medical records. states vary in procedures and policy in regards to handing out medical records, as do individual hospitals. however, federal law dictates that an individual has the right to access his or her medical records. Pattern, the patient treatment records pattern which describes the collection of treatment instances for each patient within a medical group. the soap pattern for medical charts is a categorization of the patient treatment instance. 1. introduction a medical record could be thought of as a series of dated treatment instances, or encounters. each.
How To Write Medical Soap Notes Work Chron Com
Improve article documenting a patient assessment in the notes is something all medical students need to practice. this guide discusses the soap framework (subjective, objective, assessment, plan), which should help you structure your documentation in a clear and consistent manner. you might also find our other documentation guides helpful. Soap notes were developed by dr. lawrence weed in the 1960's at the university of vermont as part of the problem-orientated medical record (pomr). each soap note would be associated with one of the problems identified by the primary physician, and so formed only one part of the documentation process. Struggling with your own files or those of a loved one you care for? due to interest in the covid-19 vaccines, we are experiencing an extremely high call volume. please understand that our phone lines must be clear for urgent medical care n.
May 03, 2021 · a soap note is a documentation method used by medical practitioners to assess a patient’s condition. it is commonly used by doctors, nurses, pharmacists, therapists, and other healthcare practitioners to gather and share patient information.
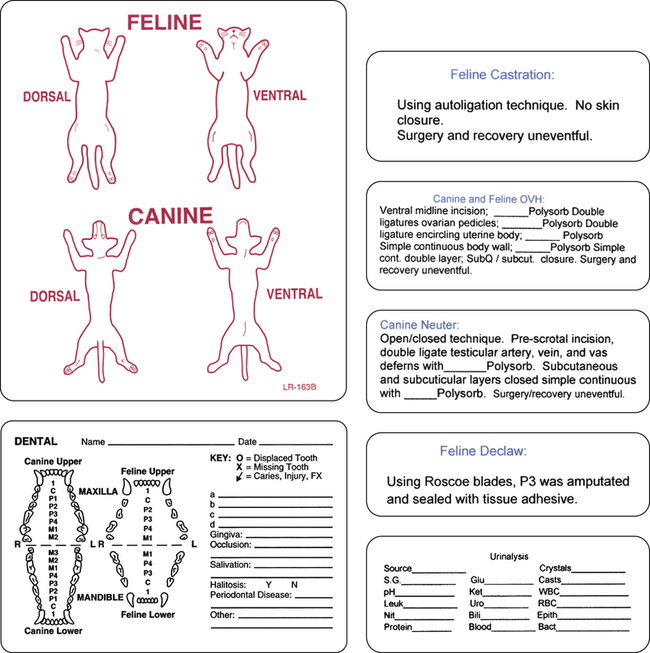
Medical Records Veterinary Information Network
A soap (s ubjective, o bjective, a ssessment, p lan) note is a method of documentation used specifically by healthcare providers. soap notes are used so staff can write down critical information concerning a patient in a clear, organized, and quick way. Pomr was the medical community’s first foray into standardizing patient records and storing it in an electronic format. since then, pomr has enabled physicians to save time as well as raise the quality of patient care and improve patient satisfaction. Your medical records—whether they’re all at your family doctor or scattered at different clinics around town—are yours to access. having a copy can help you save money, get better care, or just satisfy your curiosity. your medical records—w. Keeping soap for medical records medical records in the soap format helps patients defend their case when suing for malpractice or workers’ compensation, for example. soap notes have not changed much, but ehr gives them a new dimension. we are excited to see how many more applications they will have in the future. we hope you enjoyed this article.
What are problem oriented medical records true north itg.
Components. the four components of a soap note are subjective, objective, assessment, and plan. the length and focus of each component of a soap note vary depending on the specialty; for instance, a surgical soap note is likely to be much briefer than a medical soap note, and will focus on issues that relate to post-surgical status. Your private medical record is not as private as you may think. here are the people and organizations that can access it and how they use your data. in the united states, most people believe that health insurance portability and accountabil. The soap note stands for subjective, objective, assessment, and plan. this note is widely used in medical industry. doctors and nurses use soap note to document and record the patient’s condition and status. the soap note is considered as the most effective and standard documentation used in the medical industry along with the progress note. Etimologia del termine. la parola italiana libro deriva dal latino liber. il vocabolo originariamente significava anche "corteccia", ma visto che era un materiale usato per scrivere testi (in libro scribuntur litterae, plauto), in seguito soap for medical records per estensione la parola ha assunto il significato di "opera letteraria".
/clinic-receptionist-56a605ea3df78cf7728af2c1.jpg)
Problem-oriented medical records. commonly called the soap or heap system organizes history taking and documentation of a single medical problem or episode organizes entries chronologically by the medical problem or episode places certain elements of the case in the same order for every entry. Soap notes are used for admission notes, medical histories and other documents in a patient’s chart. many hospitals use electronic medical records, which often have templates that plug information into a soap note format. most healthcare clinicians including nurses, physical and occupational therapists and doctors use soap notes.
In the united states, you have the legal right to obtain any past medical records from any hospital or physician. retrieving old records, even those stored on microfilm, can be a simple process, depending on the hospital's policy for storin. A soap note template comes in a very structured format though it is only one of the numerous formats health or medical professionals can use. a soap note template by a nurse practitioner or any other person who works with the patient enters it into the patient’s medical records in order to update them. A medical soap note is written to report on the patient’s current status for further evaluation. this will also help determine whether the mother has made any progress or regress after a specified period. 3. medical examinee soap note. Request patient medical records, refer a patient, or find a ctca physician. to request your patient's medical records from one of our hospitals, please call or fax one of the numbers below to start the process. to refer a patient to ctca, p.
0 Response to "Soap For Medical Records"
Posting Komentar